In this post, we consider two aspects of expense for owning various dog breeds as pets—acquisition cost and estimated total cost of ownership over the expected lifespan of the dog.
The figures we’ve included are wide-ranging and perhaps not completely reliable. Click the links back to the source articles to decide for yourself.
Keep in mind, regardless of the reliability of the numbers, the estimated average expenses presented here for buying and caring for dogs of a particular breed may or may not apply to individual dogs.
The goal of our post is to provide an overview of typical costs of acquiring dogs of various breeds and help you understand health risks by exploring known health issues for the breeds you’re considering. With this information, particularly if the cost of pet ownership is an issue, you can improve your odds of spending less by choosing a breed likely to be more affordable.
What Makes a Dog Breed Expensive to Buy?
Many variables influence pricing of purebred dogs, and most breeds have a going rate range in the marketplace based on popularity, availability and breeding costs.
On a practical level, prices reflect the breeder’s out-of-pocket costs for the litter, and reputable breeders typically invest substantially more in their litters than do puppy mills and backyard breeders. In addition to food and supplies, medical exams, vaccines and deworming expenses that are typically incurred by all puppies, there could be additional expenses such as stud fees, artificial insemination costs and breed-specific genetic screening tests for the breeding stock chosen to produce a purebred litter.
At least among dog show enthusiasts, purebred pricing is influenced by the breeder’s prestige and record of producing multiple generations of winning dogs. Dogs with impressive pedigrees from leading kennels command higher prices than dogs from less prominent breeders and those not involved in competitive showing.
The most popular dog breeds are, naturally, most likely to be the most readily available, possibly—but not necessarily—at relatively affordable prices, compared with less popular and more obscure breeds. Labrador Retrievers, French Bulldogs, Golden Retrievers, German Shepherd Dogs and Poodles are likely in greater supply and perhaps more affordable than Norwegian Lundehunds, English and American Foxhounds, Belgian Laekenois and Sloughis.
For any breed, the laws of supply and demand can impact pricing and availability if a breed experiences a sudden surge of popularity because of media exposure.
Most Expensive Dog Breeds to Buy
One website we found in our research listed “20 Most Expensive Dog Breeds That Are Worth Every Penny.” The list, ordered from least to most expensive to buy, includes breeds with average estimated initial costs of $2,200 to $3,500.
The 20 breeds, listed in order of estimated average acquisition costs, include:
- Portuguese Water Dog $2,200
- Chow Chow $2,250
- Afghan Hound $2,250
- Brussels Griffon $2,300
- Saluki $2,400
- Leonberger $2,400
- Greater Swiss Mountain Dog $2,500
- English Bulldog $2,500
- English Toy Spaniel $2,500
- Giant Schnauzer $2,500
- Miniature Bull Terrier $2,500
- Nova Scotia Duck Tolling Retriever $2,500
- Azawakh $2,500
- Tibetan Mastiff $2,500
- Xoloitzcuintli $2,750
- German Pinscher $2,800
- French Bulldog $2,800
- Norfolk Terrier $3,250
- Norwich Terrier $3,500
- Neapolitan Mastiff $3,500
Besides estimated average purchase price, the article presents photographs and additional data on each of the 20 breeds, including typical height and weight ranges, personality, activity level, grooming requirements, life expectancy and average lifetime costs ranging from $14,000 to $34,000, along with summary descriptions of breed highlights.
GoBankingRates published a list of 28 most expensive dog breeds, based on estimated purchase price range, projected grooming expenses, average lifespan and potential healthcare costs for common issues faced by each breed.
Here are the 28 breeds, with estimated purchase price ranges:
- Akita $1,000 to $2,500
- Alaskan Malamute $1,200 to $2,000
- Bernese Mountain Dog $1,500 to $3,000
- Black Russian Terrier $1,000 to $2,500
- Cavalier King Charles Spaniel $1,500 to $2,500
- Chow Chow $1,200 and $2,000
- Dogo Argentino $1,500 to $2,500
- English Bulldog $2,000 and $4,000
- French Bulldog $2,000 and $4,000
- German Shepherd $800 to $2,000
- Golden Retriever $1,000 to $2,000
- Great Dane $1,000 to $2,000
- Ibizan Hound $2,000 to $2,500
- Irish Wolfhound $1,500 to $2,500
- Kerry Blue Terrier $2,000 to $2,500
- Lakeland Terrier $1,500 to $2,800
- Miniature Bull Terrier $2,500 to $3,500
- Newfoundland $1,700 to $2,500
- Old English Sheepdog $1,800 to $3,000
- Pharaoh Hound $1,800 to $2,500
- Portuguese Water Dog $2,000 to $3,000
- Rottweiler $1,200 to $2,000
- Saint Bernard $1,000 to $2,000
- Samoyed $1,500 to $3,000
- Spinone Italiano $1,200 to $2,000
- Staffordshire Bull Terrier $1,500 to $2,500
- Tibetan Mastiff $2,500 to $4,000
- Yorkshire Terrier $1,500 to $3,000
See the article for brief summaries of each breed.
Are Purebreds More Expensive Than Crossbred Dogs?
We define a purebred dog as the product of mating two dogs of the same breed. We define a crossbreed (also known as a hybrid) as resulting from a deliberate mating of two different-breed purebred dogs, such as a Cockapoo from mating a Cocker Spaniel and a Poodle, a Labradoodle from a Labrador Retriever and a Poodle or a Puggle from a Pug and Beagle mating. Technically, these are mixed-breed dogs, but in this article, when we refer to mixed-breed dogs, we’re talking about dogs of diverse parentage that most likely was not deliberately selected.
Are purebreds more expensive than crossbreds? In terms of purchase price, it appears the answer is yes.
An article at Worldofdogz.com compared purchase prices for popular purebred and crossbred dogs, demonstrating that purebreds are indeed more expensive than crossbred dogs to buy.
- The article listed these estimated price ranges for popular purebred dog breeds:
- Labrador Retriever $650 to $4,000
- French Bulldog $3,000 to $10,000
- Golden Retriever $750 to $5,000
- German Shepherd $300 to $3,200
- Standard Poodle $300 to $3,000
Average purebred price $1,000 to $5,040
For comparison, the article listed these estimated purchase prices for popular crossbred dogs:
- Cockapoo $800 to $3,200
- Labradoodle $151 to $2,000
- Goldendoodle $750 to $2,900
- Puggle $250 to $3,665
- Shepadoodle $350 to $3,000
Average $460 to $2,953
As these numbers illustrate, the crossbreds—while still potentially somewhat pricey—tend on average to be priced more affordably than purebreds.
Alternatives to Buying From a Breeder
As an alternative to buying a purebred dog from a breeder, consider adopting a purebred rescue or shelter dog.
Most dog breeds recognized by the American Kennel Club are available for adoption through the AKC Rescue Network. Locations, availability and adoption fees vary, but procuring your purebred dog through the rescue network can be a lower-cost and more satisfying alternative to buying from a breeder.
About 25 to 30% of shelter dogs are purebreds, so with patience and persistence, you may find a dog of the breed you’ve chosen at the Hendricks County Animal Shelter or Misty Eyes Animal Center.
As you plan your budget, keep in mind adoptable rescue and shelter pets have most likely already been spayed or neutered, fitted with a microchip, vaccinated, dewormed, started on parasite prevention and treated for at least the most urgent health and behavior problems presented when they arrived at the rescue organization or shelter. These initial expenses are usually covered by the adoption fee.
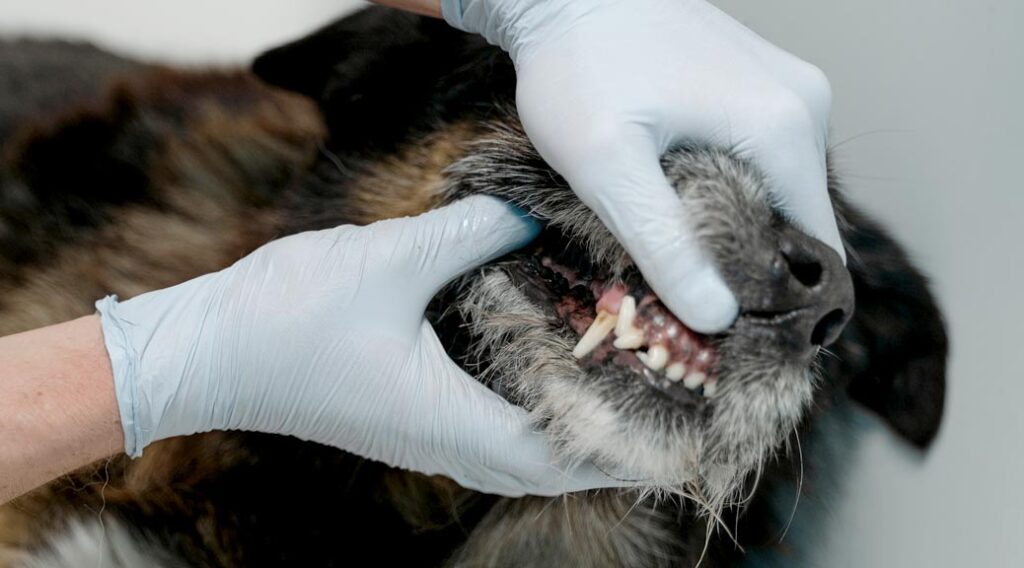
What Makes a Dog Breed Expensive to Care For?
When you choose a purebred dog, you have a good idea of its size at adulthood. As a general rule, the larger the dog, the greater the expense for feeding, equipping, grooming, boarding, insuring and providing veterinary care.
Because they are more likely to be inbred from relatively small populations, some purebred and crossbred dog breeds may be at greater risk than mixed-breed dogs for developing particular heritable health conditions. These conditions, which can be debilitating for the dog, heartbreaking for you and costly to treat, are generally well-documented for the various breeds and should be a central focus of your breed research.
For example, as a group, Cavalier King Charles Spaniels are known to be more prone than average to develop heart disease. German Shepherds have more than their share of canine degenerative myelopathy. Dachshunds have relatively more spinal issues. Boxers have an above-average incidence of cancer.
While the most reputable breeders select to improve health by screening breeding stock and attempting to eliminate defective genes, some breeders either carelessly or unknowingly disregard such considerations, and some may even select problematic traits on purpose. Bulldogs and Pugs often experience respiratory difficulties because they’re deliberately bred for their short, flat faces. German Shepherds selected for their sloping backs tend to have more hip dysplasia. Shar-Peis selectively bred for their skin folds often suffer from chronic skin infections. Such breed-specific health risks can result in higher veterinary care costs.
Health Insurance Claims by Breed
One indicator of the cost of care for dogs of various breeds is claims paid by pet health insurers. For example, based on claims filed in 2020, Embrace Pet Insurance reported the five breeds with the highest vet bills were Greater Swiss Mountain Dogs, Bernese Mountain Dogs, Flat-Coated Retrievers, Bullmastiffs and Newfoundlands.
On a more detailed short list of dogs with the highest average insurance claims, Rottweilers placed first with an average claim amount of $567.53, followed by Bernese Mountain Dogs with average claims of $412.85, Great Danes at $385.49, English Bulldogs at $370.57 and French Bulldogs at $355.63.
Another list based on insurance claims data was published by Forbes Advisor as part of a more comprehensive article on pet health insurance. On that list, the ten breeds with the highest average pet insurance claims include:
- Greater Swiss Mountain Dog $425
- Rottweiler $401
- Dogue de Bordeaux $395
- Cane Corso $386
- American Bulldog $376
- Irish Wolfhound $375
- American Staffordshire Terrier $373
- Mixed Extra Large Breeds (111 Lbs +) $368
- Bernese Mountain Dog $367
- Bull Mastiff $366
The dog breeds identified with the lowest average pet insurance claims are actually crossbreds including the Australian Labradoodle at $226, followed by the Miniature Goldendoodle at $230 and the Shichon at $241.
Bear in mind, these figures reflect individual claims amounts—not the total vet bills which would typically include the owner’s deductible and typical 20-30% share of the cost.
Least Expensive Dog Breeds
A 2021 article published on Yahoo’s finance site listed these 30 least expensive dog breeds and their estimated average purchase prices:
- Manchester Terrier $600
- Schipperke $650
- Irish Terrier $650
- German Wirehaired Pointer $700
- Border Collie $525
- Beagle $650
- Australian Terrier $550
- Pembroke Welsh Corgi $550
- Otterhound $550
- Dalmatian $700
- Chihuahua $650
- Cesky Terrier $400
- Field Spaniel $550
- Redbone Coonhound $650
- American Pit Bull Terrier $600
- Pekingese $500
- Bichon Frise $525
- Affenpinscher $400
- Dachshund $500
- Papillon $400
- Pug $350
- English Setter $350
- Treeing Walker Coonhound $500
- Miniature Pinscher $500
- American Foxhound $475
- Parson Russell Terrier $400
- Plott Hound $275
- Black and Tan Coonhound $350
- Rat Terrier $350
- Harrier $300
Visit the article to see photographs and find additional details about life expectancy, potential ailments and estimated healthcare and grooming costs for each of the 30 breeds.
Our Observations
- As noted in a previous post, the lifetime costs of owning any dog can easily amount to tens of thousands of dollars. All dogs, from the most to least expensive, need nutritious food, exercise, training, basic equipment like crates and leashes and a safe, secure environment in which to live. All dogs also need ongoing veterinary care including regular medical exams, vaccinations and parasite preventives and diagnosis and treatment of any illnesses and injuries along the way. Supplying the essentials for whatever dog you choose costs money.
- While many genetic diseases are more common in purebreds, any dog—purebred, crossbred or mixed breed—can inherit genetic diseases that disable the dog, upset you and your family and require possibly extensive, expensive veterinary care.
- Maladies associated with a particular breed will typically manifest in only a percentage of the dogs, perhaps with a higher prevalence in some bloodlines. All German Shepherds won’t necessarily develop hip dysplasia. All dogs of the Belgian breeds will not develop epilepsy. All Flat Coated Retrievers will not have cancer.
- No amount of research can predict the health outcomes of an individual dog you acquire. Doing research to determine common health problems prevalent in a particular breed will help you understand the risks associated with owning a dog of that breed, but there are no guarantees that any individual dog—purebred, crossbred or mixed-breed—will or will not experience a genetic disorder during its lifetime.
- Any dog can suffer ill health if not fed, kept safe and cared for properly. Besides providing basic food and shelter, seeking timely ongoing preventive care by our veterinarians is your best strategy for helping control the total cost of veterinary care and improving the quality of life for your dog and yourself over your dog’s lifetime.
For more information about dog breeds, visit the American Kennel Club website. Since 1884, the AKC has been registering dog breeds, keeping track of pedigrees and working with breed clubs, local kennel clubs and obedience clubs to organize dog shows year-round throughout the country. Of the 340 dog breeds known throughout the world, the AKC currently recognizes 199 breeds.